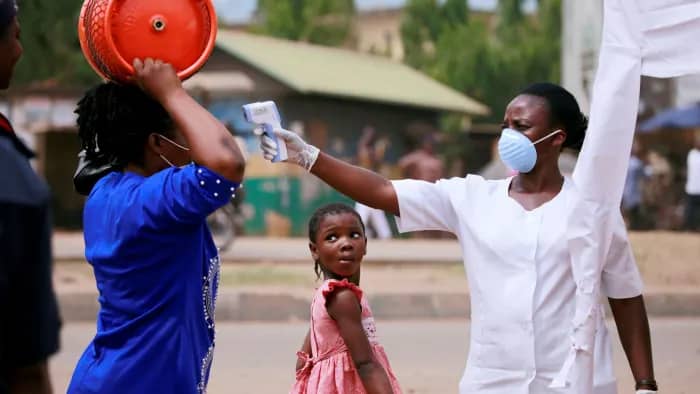African health officials have warned of a chronic shortage of the critical care equipment needed to fight coronavirus as the outbreak gathers pace on the continent.
Sierra Leone has just one ventilator for its 7.5m people. In the Central African Republic there are three machines for 5m citizens, while Burkina Faso has 11 for a population of 19m.
“There is an enormous gap in the numbers of ventilators needed,” said Matshidiso Moeti, head of the World Health Organization Africa. “And this happens in the context of a global shortage and lockdowns that will make transportation of these ventilators a challenge.”
As western countries scramble to manufacture or buy tens of thousands of ventilators to cope with the influx of coronavirus patients, it is increasingly clear that many African countries will have to make do with just a handful of the machines to help the severely ill breathe.
In Nigeria, home to the continent’s largest population, Innoson, the country’s only indigenous carmaker, has asked for a N4bn ($10.4m) government loan to repurpose its factory to manufacture the devices. But in general, experts say, there are few facilities on the continent with the potential capacity to produce the machines. International suppliers are focusing on supplying hospitals at home.
“Unfortunately, countries that used to supply us with [equipment] to fight outbreaks are also challenged,” said John Nkengasong, head of the Africa Centers for Disease Control and Prevention. “I fully understand the need for everybody to protect their citizens but this is a global challenge that requires global solidarity.”
The pandemic is in its early stages on the continent. As of Sunday, Africa had recorded just over 8,600 confirmed cases and 385 deaths. But it is tracking Europe’s trajectory and Africa CDC projects that by the end of the month a number of countries are likely to pass the 10,000-case mark.
They’re not going to be able to cope with the large numbers of people who are going to need care
David Miliband, head of the IRC
Other pieces of medical equipment are also in short supply. Countries including Burkina Faso, which has 318 confirmed cases, Cameroon, which has 555 cases, and Côte d’Ivoire, which has 245 cases, had reached out to Africa CDC to request triage tents because they were running out of hospital beds, Mr Nkengasong said.
Both the WHO and Africa CDC are working on an inventory of African countries’ capacity and needs. Some 17 governments — including Angola, Côte d’Ivoire, Mozambique and South Sudan — have told the WHO they have no intensive care unit capacity to treat severe cases of the virus.
Few African health ministries are publishing data but some international NGOs that support health systems across the continent, such as the International Rescue Committee, have made their own tallies. According to the IRC, Somalia has only 15 ICU beds for nearly 15m people, Malawi has 25 beds for 17m people and Uganda has 55 beds for 43m people.
“They’re not going to be able to cope with the large numbers of people who are going to need care,” David Miliband, head of the IRC, told the Financial Times. He said the countries had the opportunity of a few weeks to do “vital preventive work”, but added that the humanitarian community’s call for greater global funding for preventive measures in the developing world had gone unanswered.
There are some hopeful signs. Mr Nkengasong of Africa CDC lauded South Africa’s deployment of 67 mobile testing clinics and the African private sector has come forward with millions of dollars in donations.
In Nigeria, the blood delivery start-up LifeBank has opened a mobile testing unit capable of testing 200 people a day, while Co-Creation Hub, a Lagos and Nairobi-based tech incubator, is offering funding of between $5,000 and $100,000 to companies with Covid-19-related projects.
In parts of the continent dealing with violent conflicts the outlook is even worse. In northern Mali, home to a jihadist insurgency, 93 per cent of healthcare facilities have been destroyed in fighting, according to the International Committee of the Red Cross.
“The underfunded community health centres that are left already struggle to treat common illnesses like malaria and measles,” Patrick Youssef, the ICRC’s Africa director, said this week. “How could we expect them to test and treat people for Covid-19?”
Source: FINANCIAL TIMES